
Readiness Opportunity for Systems Transformation for Value-Based Care
The Centers for Medicare & Medicaid Services (CMS) Innovation Center (CMMI) launched a Request for Applications (RFA) with special considerations for rural healthcare providers traditionally unable to participate in previous Accountable Care Organization (ACO) and value-based care models. The Long-term Enhanced ACO Design (LEAD) application (https://app.innovation.cms.gov/LEAD/IDMLogin) launched March 31, 2026, and will close at 11:59 PM Eastern Time (E.T.) on May 17, 2026. The LEAD model, to run from January 1, 2027, through December 31, 2036.[1]
Per CMMI, this is the most significant ACO opportunity for rural healthcare providers in years. The LEAD model includes a 10-year performance period without rebasing and with benefit enhancements, in the form of Medicare payment rule waivers, that promote sustainable long-term benchmarks and expands covered services designed to help address geographic and workforce access barriers in rural communities.
The LEAD Model presents a transformative opportunity for rural healthcare systems to build readiness for value-based care, enhance care delivery flexibility, and improve access for underserved populations. Some of the enhanced benefits supporting rural providers include the following:
- Telehealth Benefit Enhancement expands synchronous telehealth services by waiving the geographic originating site requirements, allowing the originating site to include a beneficiary’s home, and waiving the home originating site fee requirement for services furnished by a Participant and Preferred Provider
- 3-Day Skilled Nursing Facility (SNF) Rule Waiver removes the three-day inpatient stay rule to receive Medicare-covered SNF services from qualified SNFs or swing-bed hospitals that are LEAD Participant Providers or Preferred Providers
- Post-Discharge Home Visits Benefit Enhancement provides a conditional waiver of direct supervision for certain home visits by auxiliary personnel
- Care Management Home Visits Benefit Enhancement allows for payments of certain home visits proactively provided in advance of potential hospitalization
- Home Health Homebound Waiver Benefit Enhancement waives homebound status prior to accessing home health services
- Nurse Practitioner/Physician Assistant (NP/PA) Services Benefit Enhancement allows NPs/PAs who serve as either Participant Providers or Preferred Providers expanded scope for specific care
- Concurrent Care for Beneficiaries Electing Medicare Hospice Benefit waives the requirement to give up curative care to receive the hospice benefit
- Medical Nutrition Therapy (MNT) Benefit Enhancement expanding Medicare coverage from diabetes, chronic kidney disease, and post kidney transplant to also include Pre-diabetes and Hyperlipidemia
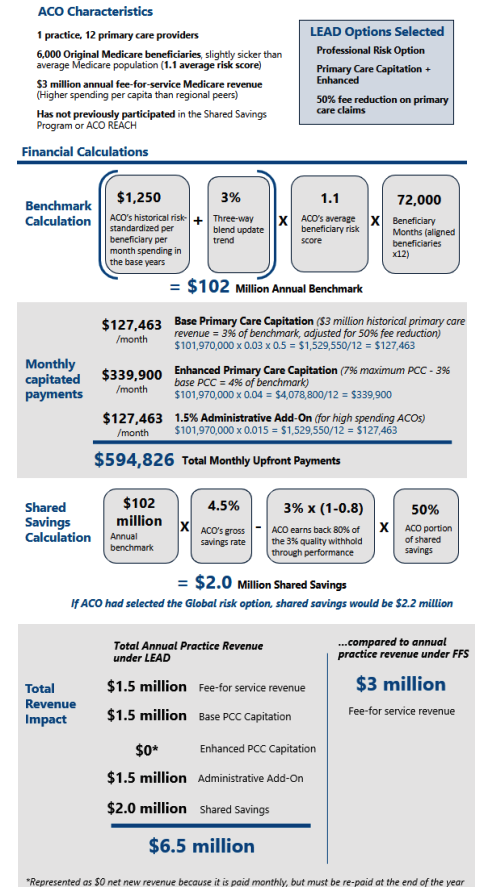
Value-Based Financial Model
The financial methodology for the LEAD Model includes flexible risk-sharing options, benchmarking approaches, risk mitigation strategies, timely financial settlements, and payment mechanisms designed to support both new and experienced Accountable Care Organizations (ACOs).
Risk-Sharing Options
The model offers two distinct risk tracks based on Medicare Total Cost of Care (TCOC):
- Global Risk Option: ACOs assume 100% of savings and losses
- Professional Risk Option: ACOs share 50% of savings and losses with CMS
(See Appendix for CMMI demonstration scenarios illustrating potential Global and Professional risk outcomes.)
- Benchmarking methodology including adjustments for lower and higher spending ACOs, and separate per-beneficiary per-month benchmarks for three beneficiary categories: Aged & Disabled, End-Stage Renal Disease, and High Needs. The CMMI also includes considerations specifically for Rural Health Centers and Federally Qualified Health Centers (RHCs and FQHCs) totaling up to a 3% savings “wedge” to be shared by the ACO and Medicare.
- Risk mitigation where savings or losses that ACOs in the Global or Professional Risk Options realize will be constrained by a series of risk corridors.
- Financial settlements include the options between the Provisional Financial Settlement for more timely payments, and the Final Financial Settlement which includes claims run-out.
- Payment mechanisms and claims reductions untangle payments with Medicaid fee for service for certain services, and provides steady, predictable cash flow. Services subject to payment reductions are based on the capitated payment option and reduction percentage selected by the ACO. The CMS reports that this flexibility frees health care providers to deliver care in innovative and flexible ways, such as non-face-to-face care management, telehealth, and electronic messaging, without worrying about foregoing fee-for-service revenue.
Financial Protections for Rural Safety-Net Providers
The CMMI highlights that the LEAD Model includes significant financial protections for rural healthcare safety-net providers. Federally Qualified Health Centers (FQHCs) and Rural Health Centers (RHCs)—which operate under alternative reimbursement methodologies—benefit from a base capitated payment “true-up” through the following mechanisms:
- Quarterly Revenue Reconciliation: Payments are assessed on a year-to-date basis, with any shortfalls corrected on a quarterly basis
- One-Directional Capitation Adjustments: Adjustments can only increase payments, ensuring no downside financial risk from capitation
- Alignment with Value-Based Measures: Quality measures apply across all beneficiaries aligned through FQHCs and RHCs within the ACO
- Elimination of Underpayment Risk: The true-up mechanism mitigates the financial risk of underpayment under capitated models
Continuous Quality Improvement
The LEAD Model incorporates a value-based methodology centered on seven clinical quality benchmarks spanning claims, patient experience surveys, and Electronic Clinical Quality Measures (eCQMs). The CMS reports that these measures were selected based on clinical impact, actionability, and alignment with CMMI priorities, with CMS reserving the right to update measures and scoring annually.
Opportunities for incentive payments and bonuses are tied to sustained quality performance. Initial quality measures include:
- Risk-standardized all-cause readmissions within 30 days of discharge
- All-cause unplanned admissions among beneficiaries aged 66+ with multiple chronic conditions
- Days at home for patients with complex, chronic conditions
- Timely follow-up after acute exacerbations (e.g., hypertension, asthma, heart failure, COPD, diabetes)
- Patient-reported outcomes via the ACO CAHPS survey composite score
- Controlling high blood pressure
- Glycemic status assessment for patients with diabetes
Additionally, ACOs are also required to develop a Prevention and Quality Plan (PQP) outlining strategies across the full continuum of care, from primary to tertiary prevention. The PQP will be implemented in phases:
- Phase 1: Program Year 1
- Phase 2: Program Year 2
- Phase 3: Program Years 3–10
The CMS will directly tie payments to both the development and successful execution of PQP goals.
Building an Accountable Care Organization through the Hub-and-Spoke Model
The LEAD model promotes the CMS goal of aligning all Medicare and most Medicaid payments with value-based payment models by 2030.[2] Success in the LEAD model is dependent upon the strength of the infrastructure, processes, and connectivity of the ACO. Rural healthcare providers are again strongly encouraged to join a Hub and Spoke model, form relationships that re-organize independent organizations into multi-specialty robust healthcare systems and strengthen all participating partners via shared costs and resources.
This model is also supported by the Substance Abuse and Mental Health Services Administration (SAMHSA) as an effective framework for expanding access to substance use disorder (SUD) and mental health treatment.[3] The SAMHSA’s “no wrong door” approach supports the needs of individuals living with mental health and/or substance use challenges via assessment, intervention, and coordination of care via all ACO touch-points.
Technology Requirements
The LEAD model also includes a requirement for all providers to leverage Certified Electronic Health Record Technology (CEHRT). When there exists clinicians who require temporary exceptions, CMS will include a one-year CEHRT transitional pathway (exceptions may be extended subject to CMS discretion). Additionally, LEAD will include a three-year CEHRT deferral for providers with advanced, custom, or home-grown health IT systems, providing more time to adopt CEHRT.
We Are Here to Help
SunHawk provides expertise in readiness reviews and assists rural healthcare providers in successful participation in LEAD models.
To support readiness, SunHawk has developed a comprehensive checklist (download here) to help organizations assess their preparedness and strategic alignment with the Request for Applications (RFA).
Partner with SunHawk to:
- Conduct application readiness review
- Evaluate value-based care readiness
- Design ACO infrastructure and process flows
- Analyze revenue cycles, including identifying leakage
- Assess Electronic Health Record (EHR) compliance
- Identify high-volume patients for CMS benchmarking categories
- Detect missed coding opportunities
- Identify and engage unattached patients
[1] Centers for Medicare and Medicaid, LEAD (Long-term Enhanced ACO Design) Model, Request for Applications, March 31, 2026, https://www.cms.gov/priorities/innovation/innovation-models/lead
[2] Centers for Medicare and Medicaid, CMS Moves Closer to Accountable Care Goals with 2025 ACO Initiatives, Newsroom, January 15, 2025, https://www.cms.gov/newsroom/fact-sheets/cms-moves-closer-accountable-care-goals-2025-aco-initiatives
[3] Substance Abuse and Mental Health Services, 2025 National Guidelines for a Behavioral Health Coordinated System of Crisis Care, January 15, 2025, https://library.samhsa.gov/sites/default/files/national-guidelines-crisis-care-pep24-01-037.pdf
[4] Centers for Medicare and Medicaid, LEAD (Long-term Enhanced ACO Design) Model, Request for Applications, March 31, 2026, https://www.cms.gov/priorities/innovation/innovation-models/lead
Appendix
Global Risk Option: Designed for ACOs Experienced in Value-Based Care [4]
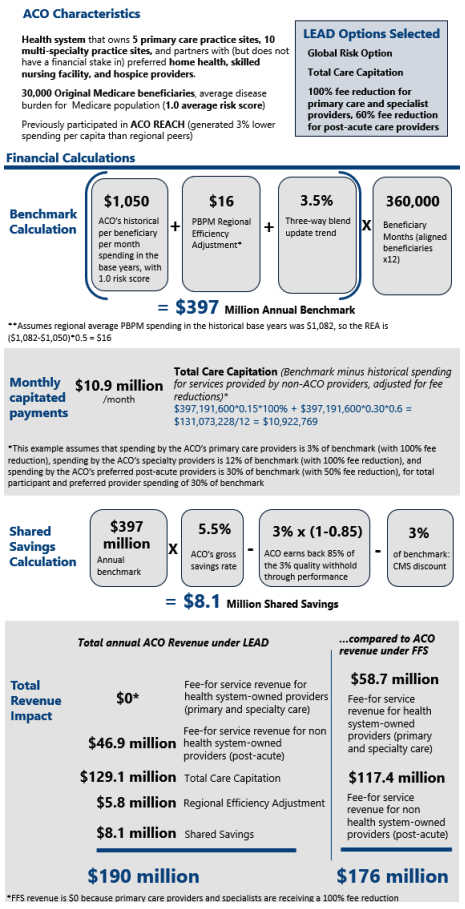

Professional Risk Option: Designed for ACOs New to Value-Based Care

Brigita Landstrom, MHS, CPHQ, CAS
Director
SunHawk Consulting
Brigita Fody Landstrom has 25 years of Medicare/Medicaid managed care, Community Health Center Quality, and large hospital and healthcare systems experience. Passionate about population health, Brigita has dedicated her career to serving the health of communities, with extra attention on traditionally marginalized populations. Brigita has worked with leaders and regulators within multiple market segments on data-driven systems improvement, large-scale health program implementation, grant writing, risk contracting, budget development, policy development, and staff training and support.

Sailaja Prakriya
Director
SunHawk Consulting
Sailaja Prakriya is a healthcare analytics and transformation leader with more than 20 years of experience helping payer, provider, and government healthcare organizations improve operational performance, financial outcomes, and population health through data-driven strategies. She specializes in healthcare analytics strategy, revenue cycle performance analytics, and value-based care transformation, helping organizations translate complex healthcare data into actionable insights that drive measurable improvement.
SunHawk experts are highly experienced professionals ready to assist you within our focus areas of:
Healthcare Compliance | Corporate Investigations
Corporate Compliance | Litigation Disputes
Have a question? We are ready to answer it.
