
The Centers for Medicare & Medicaid Services (CMS) Rural Health Transformation Program (RHTP) is designed to address critical provider shortages in rural communities driven by hospital and clinic closures, workforce attrition to urban areas, and persistent recruitment challenges. Simultaneously, CMS is accelerating the transition to value-based care, with a goal of aligning all Medicare and most Medicaid payments with alternative payment models by 2030.[1]
Rural populations continue to experience disproportionately high unmet physical and behavioral health needs, compounded by geographic, economic, and infrastructure barriers. In response, RHTP promotes the development of Hub and Spoke care delivery models to stabilize access, expand services, and improve health outcomes across rural regions.
This model is also supported by the Substance Abuse and Mental Health Services Administration (SAMHSA) as an effective framework for expanding access to substance use disorder (SUD) treatment. By embedding care managers and navigators and implementing a “no wrong door” approach, the model ensures patients receive comprehensive, coordinated care regardless of entry point.
The Hub and Spoke Model: A Framework for Rural System Transformation
The aim of Hub and Spoke models is to re-organize independent organizations into more robust healthcare systems that reduce per patient costs and strengthen all participating partners via shared costs and resources. The Hub and Spoke models’ improvement goals include:
- Interoperable Coordinated Care: Integrates primary care with multidisciplinary teams, enhancing patient-centered care, reducing administrative burdens, avoidable emergency department visit, and hospitalizations, and closing gaps in value-based care measures.
- Flexible Healthcare Entry: ensuring primary healthcare and specialty healthcare for patients in rural areas based on patient needs and preferences, including in-person, virtual visits, and satellite/mobile services.
- Efficacious Delivery: services provided based on scope and coordination, including hospitals serving as hubs for high-risk, high-cost procedures and local clinics providing essential primary mental and physical healthcare, and routine lower-cost services via local providers.
- Sustainability and Scalability: reduced per patient costs allows for the stabilization of the entire system and provides the backing essential for any needed expansion of services.
- Workforce Development: creating multidisciplinary teams with opportunities for internships, residency programs in mental and physical healthcare, and learning collaboratives.
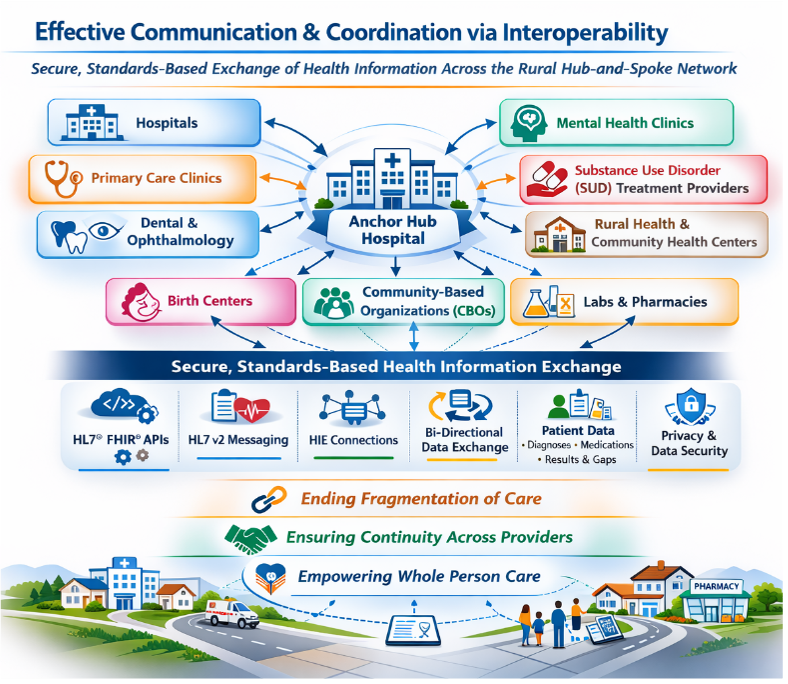
Effective Communication and Coordination via Interoperability
Interoperability is the heart of seamlessly linking separate rural provider IT systems, devices, and electronic medical records to provide informed care. This linkage removes fragmentation, avoids duplicate or missing services, and provides every provider with the information needed to successfully close or schedule care to address value-based performance indicators.
Specifically, Interoperability refers to the secure exchange and use of electronic health information across organizations and systems through standards-based approaches, including HL7® FHIR® (Fast Healthcare Interoperability Resources) application programming interfaces (APIs) and other established health data exchange methods like:
- HL7 v2 messaging
- C-CDA documents
- HIE connections
- payer-provider exchange
- referral platforms
- ADT feeds
- lab/pharmacy/result interfaces
The HL7 FHIR standards to securely and seamlessly exchange electronic health information to all providers in the Hub and Spoke system by leveraging secure web technologies like HTTP, RESTful APIs, and JSON/XML to share critical patient data (diagnoses, medications, healthcare gaps, test results, etc.) timely and effectively resulting in empowering all provider touchpoints to actively promote whole person care. Of import, the model advances real-time bi-directional communication between and within the Hub (anchoring hospital) and Spokes (local mental and physical healthcare provider) reducing administrative burden and allowing for seamless between all providers maintaining continuity of care.
Rural Healthcare Hub and Spoke Model
Truly integrated, this model strengthens rural communities by creating coordination between all provider touchpoints (with appropriate privacy controls), facilitating “no wrong door” for essential care.
- Hospitals
- Primary Care Clinics
- Dental & Ophthalmology
- Mental Health Clinics
- Federally Qualified Healthcare Centers
- Rural &Community Health Centers
- Substance Use Disorder Treatment Providers
- Birth Centers
- Community Based Organizations
- Labs & Pharmacies
- Registered Dieticians
- Skilled Nursing Facilities
- Mobile & Satellite Health Clinics
- School-based Health Clinics
- Physical & Occupational Therapy
- Street Medicine
The “no wrong door” approach ensures every patient interaction is maximized to close care gaps, promote whole-person healthcare, and meet RHTP value-based performance metrics. SunHawk’s experts in interoperability and rural health care can demonstrate how rural healthcare systems can achieve outcomes, optimize resources, and improve long-term sustainability.
Innovation Spotlight
Expanding Access to Primary Care in Rural Communities, the Hybrid Approach
EnlightenMed increases access and advance care in rural and underserved communities through hybrid telemedicine blending in-person clinical presence with virtual care delivery to meet patients where they are, without sacrificing the continuity and relationship that rural medicine demands.
EnlightenMed includes multidisciplinary teams, such as primary and specialty care physicians, advanced practice providers, nurses, health coaches, and digital health navigators which carry dedicated patient panels, functioning as a medical home within the community. Every member of the care team carries behavioral health training, offers five-year contracts, and provides supervision for local clinical interns.
Interoperability in Action
The EnlighenMed platform integrates directly into the existing EHR systems through industry-standard FHIR APIs to avoid duplication documentation and parallel workflows. Two core programs help manage the highest-risk patients while unlocking alternative payment revenue streams include:
- Advanced Primary Care Management (APCM) serving complex patients, closing care gaps, and generating structured monthly reimbursement between visits.
- Remote Patient Monitoring (RPM) extending the clinic into the home, capturing real-time vitals and triggering interventions to help avoid emergency visits or readmissions.
The RHTP and CMS quality programs all reward the same thing, measurable outcomes. Reduced readmissions. Improved chronic disease metrics. Documented health equity. EnlightenMed delivers those outcomes and documents them in ways that satisfy state and federal reporting requirements. EnlightenMed was built from the inside out. Our founders practiced rural medicine firsthand, lived in the communities they served, and understood that the problem was never the people delivering care. It was the infrastructure around them.
SunHawk Consulting – We Can Help
SunHawk consultants bring more than 20 years of experience supporting Rural Health Clinics (RHCs), Critical Access Hospitals (CAHs), Federally Qualified Health Centers (FQHCs), Community Health Centers (CHCs), School-Based Health Centers (SBHCs), primary care practices, behavioral health providers, and other rural organizations in developing and strengthening integrated care models.
Our expertise supports rural providers in delivering essential, high-quality care within their communities.
Examples of Our Services:
- Grant proposal writing and strategy
- Substance use and co-occurring disorder program development
- Integrated behavioral and primary care model implementation
- Quality Assurance and Performance Improvement (QAPI) program development and evaluation
- Compliance program development and auditing
- Project and program management
- Healthcare information management and medical records optimization
- Healthcare compliance, privacy, and security programs
- Governance support and interim leadership
Contact us to learn how SunHawk can help you leverage RHTP opportunities to strengthen long-term financial sustainability while improving clinical quality and community outcomes. We’re ready to support your strategic planning and implementation needs.

Brigita Landstrom, MHS, CPHQ, CAS
Director
SunHawk Consulting
Brigita Fody Landstrom has 25 years of Medicare/Medicaid managed care, Community Health Center Quality, and large hospital and healthcare systems experience. Passionate about population health, Brigita has dedicated her career to serving the health of communities, with extra attention on traditionally marginalized populations. Brigita has worked with leaders and regulators within multiple market segments on data-driven systems improvement, large-scale health program implementation, grant writing, risk contracting, budget development, policy development, and staff training and support.

Sailaja Prakriya
Director
SunHawk Consulting
Sailaja Prakriya is a healthcare analytics and transformation leader with more than 20 years of experience helping payer, provider, and government healthcare organizations improve operational performance, financial outcomes, and population health through data-driven strategies. She specializes in healthcare analytics strategy, revenue cycle performance analytics, and value-based care transformation, helping organizations translate complex healthcare data into actionable insights that drive measurable improvement.
SunHawk experts are highly experienced professionals ready to assist you within our focus areas of:
Healthcare Compliance | Corporate Investigations
Corporate Compliance | Litigation Disputes
Have a question? We are ready to answer it.
